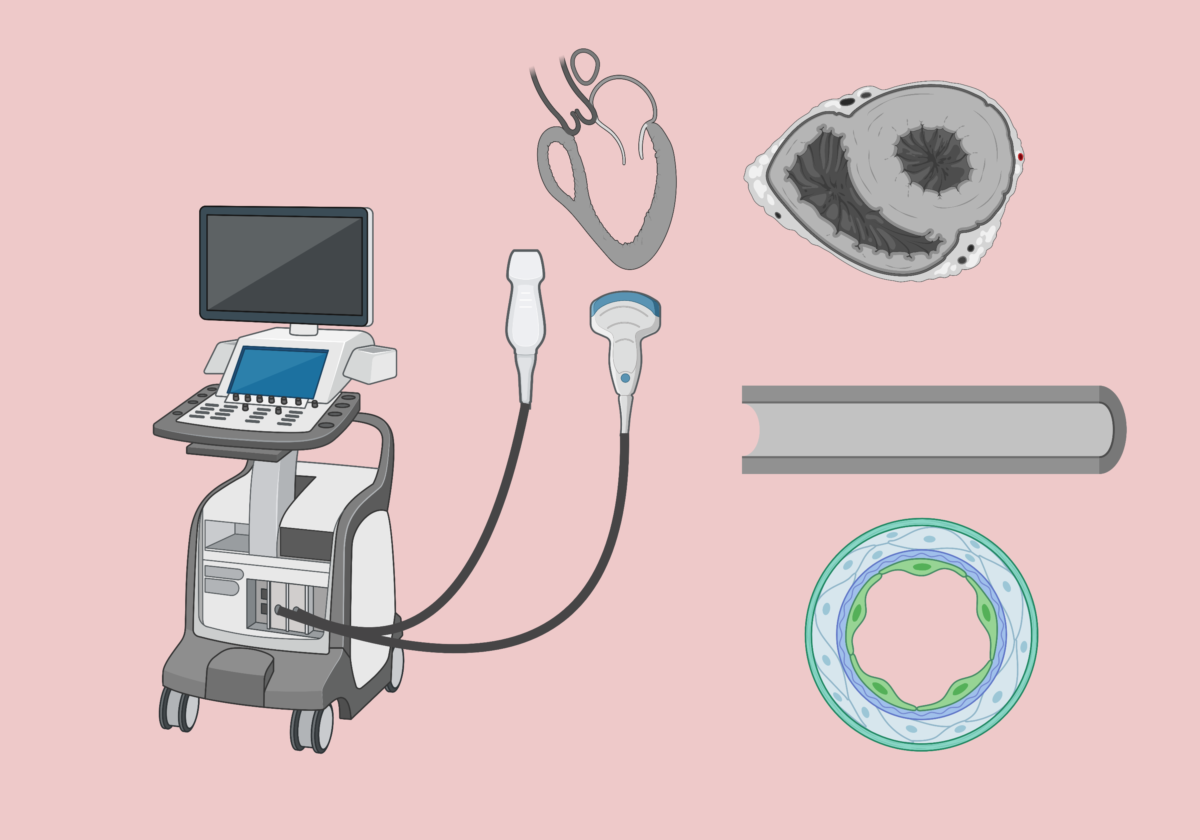
In emergency situations, particularly when treating pets in shock, quickly assessing left ventricular (LV) function is crucial for determining the best course of action and accurately diagnosing the type of shock (cardiogenic vs. hypovolemic vs. distributive vs. obstructive). A fast, reliable method that emergency veterinarians can use is Point-of-Care Ultrasound (POCUS in dogs and cats with shock). This “eyeball” approach allows us to evaluate LV contractility efficiently.
In this post, I’ll walk you through the three primary components of LV function assessment using POCUS, which can be easily applied by non-cardiologists. By mastering these techniques, you’ll be able to identify whether your patient’s LV function is hyperdynamic, normal, or depressed in just a few moments.